
Bronchitis and Emphysema: "COPD"
WHY ARE BRONCHITIS AND EMPHYSEMA CONSIDERED TOGETHER?
Chronic bronchitis and pulmonary emphysema are the main causes of respiratory disability in the United States. They account for over 50,000 deaths each year. Between five and ten million Americans are partially or totally disabled from these conditions. Because the diseases share many common characteristics, they are often referred to as chronic obstructive pulmonary disease or COPD for short. (Some physicians use the term chronic obstructive lung disease or COLD; since this can be confused with the common cold, COPD is the preferred abbreviation).
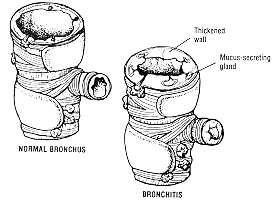
Chronic bronchitis and emphysema are due mainly to longterm cigarette smoking. In both conditions there is damaged airways and patients experience shortness of breath. Figure 1 illustrates how most physicians view the two conditions. Although there are specific differences, and some patients have predominantly chronic bronchitis or emphysema, most patients suffering from "COPD" have elements of both.
To put these diseases in perspective, questions on
bronchitis will be answered first, followed by questions on emphysema.
Keep in mind the common cause (smoking) and clinical overlap in
most cases.
WHAT IS BRONCHITIS?
Bronchitis is inflammation of the airways of the lungs that leads to increased mucus production, making people cough. It can occur in various forms but is usually divided into "acute" and "chronic." In acute bronchitis you feel very sick and have a hacking cough; this is usually accompanied by fever and flu-like symptoms. In the chronic form you cough up mucus daily for at least several months each year but do not feel acutely ill. People with chronic bronchitis are usually able to work unless the disease is far advanced. Because everyone coughs sometimes, the medical definition for chronic bronchitis requires daily cough and mucus production for at least three months of the year for two consecutive years.
Acute bronchitis is usually due to a virus or bacterial infection; the infecting organism settles in the airways and leads to inflammation and increased amounts of mucus production. Acute bronchitis may occur in nonsmokers as well as in patients with COPD. Treatment with antibiotics usually leads to recovery within a few days, unless there is a complication.
Chronic bronchitis is most commonly due to cigarette smoking, although there are other causes (see next section).

IS CHRONIC BRONCHITIS JUST A "REACTION" TO IRRITANTS, OR IS IT A SPECIFIC DISEASE?
Chronic bronchitis is a reaction of the airways to
irritants. It can also be called a disease but one with many possible
causes. Regardless of the cause the symptoms are usually the same:
chronic cough and expectoration of mucus. Cigarettes, the principal
cause of chronic bronchitis, probably act via the "tar"
in the smoke; "tar" irritates the airways and damages
the ciliary clearance mechanism, impairing the lungs' ability
to handle mucus. People who have never smoked can still develop
chronic bronchitis. Some conditions that can cause chronic bronchitis
in nonsmokers include:
Cystic fibrosis (CF) is an inherited disorder that usually appears in childhood and affects mucous secretions in the lungs, pancreas, and other organs. CF patients almost always have chronic cough.
Chronic, under treated asthma can lead to chronic bronchitis and be indistinguishable from COPD seen in smokers.
Chronic bronchitis patients also have an increased
risk of developing acute bronchitis. Thus, acute bronchitis can
occur on top of chronic bronchitis. (People without chronic
bronchitis can also contract acute bronchitis; but it's usually
of short duration. By contrast, patients with chronic bronchitis
may suffer frequent attacks of acute bronchitis.) The condition
may progress even further to pneumonia, which is infection of
the smallest air spaces (alveoli) in the lungs.
WHAT IS THE NATURAL HISTORY OF CHRONIC BRONCHITIS?
Natural history refers to the usual or expected course
of a disease. For chronic bronchitis, as with so many lung diseases
except perhaps lung cancer, the natural history is highly variable.
One can have mild, moderate, or severe disease. Generally, the
longer the symptoms have been present and the longer the exposure
to cigarettes (or whatever cause), the more severe will be the
disease. However, there is great individual variation. For this
reason physicians frequently order breathing tests (pulmonary
function tests) on patients with suspected COPD. These tests of
lung function require the patient to exhale quickly and forcefully
through a tube attached to a measuring device. Another test, blood
gas analysis, is performed on a sample of arterial blood and determines
if the patient's lungs are bringing in enough oxygen and getting
rid of enough carbon dioxide. These tests (pulmonary function
and arterial blood gas) give the best idea of disease severity
and what the longterm outlook may be.
HOW DOES CIGARETTE SMOKE CAUSE CHRONIC BRONCHITIS?
Healthy lungs produce mucus constantly. It comes from the millions of cells that make up the lining of the airways, and forms a "blanket" layer inside the airways. Underneath this blanket are cilia, tiny hairs that act in unison to move the mucus blanket up the airways to the throat, where the mucus is swallowed. This is possible because the trachea (the large air tube in the neck) and the esophagus (which leads to the stomach) share a common passage in the back of the throat.
This mucus blanket effectively gets rid of the everyday air pollutants and dusts we inhale. If the dust is not excessive our lungs won't become damaged and the normal defense mechanisms won't be overcome. However, when cigarette smoke or another pollutant is constantly inhaled the ciliary action will become impaired. Inhalation of cigarette smoke over a long period of time can destroy the ciliary blanket. When that happens the cilia don't beat normally; in some cases the cells lining the airways are also destroyed so that the lining is denuded. Without a normal ciliary mechanism mucus won't be swept out; increased mucus secreted in response to inhaled pollutants won't be cleared. The result is a chronic, daily cough.
In the mildest cases mucus may be coughed up in the
morning and either swallowed or expectorated by the patient; this
is known as morning cough or in some cases smokers' cough. If
the condition persists throughout the day, it is a chronic smokers'
cough. In the most severe cases the airways themselves are permanently
damaged, beyond any natural healing process, and the patient then
has one type of chronic obstructive pulmonary disease: chronic
bronchitis (see Figure 2).
WHAT IS ASTHMATIC BRONCHITIS?
In many case chronic bronchitis blends in with asthma
(see Section E). First, patients with chronic bronchitis may develop
an asthma syndrome. Second, patients with longstanding asthma
may develop chronic mucus production and chronic bronchitis. In
either case the resulting condition is referred to as asthmatic
bronchitis. (Interestingly, chronic asthma does not lead to emphysema—unless
the patient smokes.) Although most cases of COPD are due to cigarette
smoking, the cause of asthma is unknown.
Patients with predominant emphysema may also develop
an asthma-like picture. Since asthma is a reversible condition,
the same asthma drugs are commonly used to treat COPD patients,
with the goal of reversing whatever airway narrowing will respond.
With this concept we can expand our twocircle diagram to
three circles, as shown in Figure 3.
HOW IS CHRONIC BRONCHITIS TREATED?
There are several therapeutic modalities for treating
chronic bronchitis, but not all are used simultaneously in every
patient. The only one that should be universally applied to every
patient is "stop smoking or never start." This and other
modalities are listed in Table 1.

| Stop Smoking - Almost all patients with chronic bronchitis are or have been cigarette smokers. |
| Avoid Passive Smoke - This is particularly true if a spouse smokes around the patient. |
| Bronchodilators - These are drugs designed to open up the airways. See Section E. |
| Steroids - These drugs, such as prednisone, are very helpful in some severe cases of chronic bronchitis, especially when there is an asthmatic component. See Section E. |
| Antibiotics - These are widely used for exacerbations of chronic bronchitis. |
| Oxygen - This is reserved for the sickest, usually hospitalized, patient. See Section P. |
| Chest Physical Therapy - This form of treatment attempts to mobilize secretions by mechanical (percussing the back) and gravitational methods (postural drainage). It is used mainly in hospitalized patients. Although its efficacy is not proven, many physicians and patients feel it is beneficial. |
Patient John T. – A Case of Severe Chronic Bronchitis
Mr. T. is a 57yearold car salesman who has had a hacking cough and a low grade fever for several days. Except for several colds a year he has enjoyed good health. He has a long history of cigarette smoking, at least a pack a day since age 17. He also admits to having a daily morning cough that brings up small amounts of whitish sputum; this has been going on for several years and has never bothered him – in fact he considers it normal. His current cough is much different in its intensity and in the color of the sputum produced – now it is greenishyellow.
Examination of his chest with a stethoscope reveals a few wheezes. A chest X-ray is negative – no abnormal shadows are seen. The negative Xray helps to rule out pneumonia or lung cancer as the cause of his current problem. His sputum, examined under the microscope, shows many bacteria. The diagnosis of acute bronchitis is made and Mr. T. is given a prescription for ampicillin, an antibiotic. He is also told in no uncertain terms to quit smoking.
Four days later he is better and able to return to work. He notices, however, some shortness of breath after exertion, such as climbing stairs, a symptom not present before his acute illness. Although he does not resume smoking, his breathing problem persists, and pulmonary function tests are ordered.
In the pulmonary function laboratory Mr. T. undergoes both a blood test and spirometry. First, an arterial blood sample is drawn and analyzed for carbon dioxide, oxygen tension, and blood acid levels. Next, he is asked to breathe in deeply and blow all his air out into a hose connected to a spirometer. This test is repeated after he has inhaled some medication used to open up the airways.
The test results are abnormal. The blood test shows that, while he is ventilating adequately (at rest he is moving enough air in and out of his lungs) and has normal blood acidity, he is not transferring oxygen into his blood properly; his blood oxygen tension is lower than it should be. The spirometry test shows he has airway obstruction – he cannot blow the air out as fast as normal men his age. In addition, the medication has no effect in opening up his airways.
These tests, plus his history, confirm the diagnosis of COPD and chronic bronchitis. The chronic bronchitis is due to cigarette smoking and at this point is not reversible. The airways, were they examined under a rnicroscope, would show abnormal thickening and swelling due to repeated insults from cigarette smoke.
Although he claims no symptoms before
his episode of acute bronchitis, his history suggests chronic
bronchitis for many years. Had breathing tests been done a year
earlier they would have shown airway obstruction also, though
perhaps less severe. When he developed acute bronchitis he was
at the threshold of symptoms; the acute infection "tipped"
him over and now he notices his pulmonary impairment (see Figure 4). Normal lung function will not return, and continued smoking
will only hasten lung destruction, perhaps causing emphysema as
well (not yet evident). Hence, complete cessation of smoking is
a critical part of his medical management. In addition, Mr. T.
will receive antibiotics at the first sign of another acute lung
infection. Fortunately, his blood oxygen tension is not low enough
to warrant home oxygen therapy and his lung disease is not endstage.
He has a moderate case of COPD and with good medical management
may continue to work until retirement.
WHAT IS THE VALUE OF BREATHING TESTS IN COPD?
The case of Mr. T. illustrates how a patient can smoke for years and "suddenly" develop symptoms. In fact, COPD develops over many years, yet shortness of breath occurs only late in the course. Figure 4 illustrates what happens. Breathing tests begin to fall below normal, but initially the patient has no symptoms. Then with a little further decline in lung function, the patient notices shortness of breath. Because the symptom "shortness of breath on exertion" appears to have come on suddenly, the decrease appears acute; in fact, the underlying airway damage builds over years and continues until the threshold of symptoms is finally reached.
Although not everyone's threshold for developing
symptoms is the same, most COPD patients will have years of gradually
decreasing lung function before they feel short of breath.
Thus breathing tests can help detect and measure this impairment
before it is too late.
Figure 4. Decline of lung function in patients
with chronic obstructive pulmonary disease (COPD). Patients do
not suddenly develop COPD. As shown here lung function declines
over many years. When the threshold for symptoms is reached (shown
at 50% of lung function in this figure – the
exact point will vary among individuals), the patient notices
shortness of breath. Lung function may continue to decline, leading
to progressive worsening of symptoms.

WHAT IS THE DIFFERENCE BETWEEN CHRONIC BRONCHITIS AND EMPHYSEMA?
Although both diseases are caused by cigarette smoke,
the damage in the two cases is different. Chronic bronchitis starts
with ciliary damage; in the most severe cases the airways themselves
are irreversibly damaged, yet the basic architecture of the lungs
remains intact. In emphysema not only are the airways damaged,
but many of the alveoli and their accompanying blood vessels are destroyed. They are destroyed
by the effects of the cigarette smoke, leaving only empty air
spaces that cannot effectively transfer oxygen and carbon dioxide.
For gas exchange to occur the patient has to literally work harder
to bring more air into the remaining normal air spaces. For this
reason emphysema is generally a more severe condition than chronic
bronchitis, and not usually amenable to any specific treatment.
Figure 5 diagrams the basic differences in airway structure between
the two conditions.
Figure 5. Two alveoli from a normal lung and from
lungs involved with chronic bronchitis and emphysema. Blood vessels
are not shown in this figure. In chronic bronchitis the airways
are narrowed but intact. In emphysema the damage is more extensive,
involving actual destruction of alveoli and blood vessels; note
the coalescence of two alveoli into one larger, ineffectual "space"
that no longer functions as a normal alveolus. The end result
in chronic bronchitis is thickened air tubes and loss of the ciliary
blanket. The end result in emphysema is literally "holes"
in the lung.

WHY DO SOME CIGARETTE SMOKERS DEVELOP CHRONIC BRONCHITIS AND OTHERS EMPHYSEMA?
As stated earlier, most patients who contract chronic obstructive lung disease have elements of both chronic bronchitis and emphysema, although one or the other may dominate in a given individual; physicians can usually determine which process predominates.
Chronic bronchitis is found most commonly in patients who have inhaled tremendous amounts of cigarette smoke; the "tar" has had a direct, toxic effect on their bronchi. It's possible that anyone inhaling comparable amounts of smoke would have similar changes. This doesn't rule out a genetic or constitutional factor, but the end result (chronic bronchitis) does seem related to the dose of toxic material ("tar") inhaled.
Patients who develop predominant emphysema, where the lung tissue is destroyed, may have a genetic or constitutional basis. Certainly most smokers don't develop emphysema. Evidence for a genetic tendency comes from the small percentage of emphysema patients who lack a certain enzyme called alphalantitrypsin. This enzyme, normally present, functions to break down another enzyme (trypsin) that tends to destroy lung tissue. If trypsin accumulates, as it might with alphalantitrypsin deficiency, the result can be lung destruction (emphysema). Perhaps they have some other yet-to-be discovered genetic deficiency.
Deficiency of alphalantitrypsin is an inherited disorder present in less than two percent of the population. Fortunately, this deficiency itself rarely causes severe lung disease unless the patient smokes. There is a synergistic effect between this inherited deficiency and cigarette smoke, presumably leading to destruction of the lung tissue by the body's enzyme system. Although this helps to explain why some people get emphysema, it does not explain all or even most cases. The vast majority of emphysema patients do not lack alphalantitrypsin.
It is likely that other (so far unknown) factors
will explain why some cigarette smokers develop emphysema, other
smokers chronic bronchitis, and still other smokers no major impairment
at all. (Similar information may help explain why only some smokers
get lung cancer.) If such highly susceptible people could be identified
early in their smoking career (or before they begin), this information
might be an incentive to stop smoking.
CAN INHALING PASSIVE SMOKE CAUSE COPD?
The evidence that passive smoke can cause lung cancer
and chronic pulmonary disease seems to be increasing yearly. It
is now thought that people who inhale only other people's smoke
can develop chronic lung disease over a period of time.
We have seen several non-smoking women, whose husbands smoked
heavily, develop COPD. We have also seen COPD in non-smokers who
worked in bars for a long period of time, where cigarette smoke
is usually very thick. However, inhaling passive smoke for brief
periods should not cause significant lung disease unless there
is an asthmatic-type reaction.
WHAT ARE THE SEVERE EFFECTS OF CHRONIC BRONCHITIS AND EMPHYSEMA?
The major symptom of either chronic bronchitis or
emphysema is difficulty breathing, or shortness of breath. If
this occurs only on heavy exertion, most people are able to live
comfortably. However, in some patients shortness of breath occurs
with the slightest effort or even at rest! These people, severely
limited, may require daily medication and continuous oxygen therapy.
The endstage of these conditions is known as
respiratory failure, a failure of the lungs to bring in oxygen
and get rid of carbon dioxide in an efficient manner. Some patients
are still able to adapt if the respiratory failure is chronic
and they have had time to adjust. When respiratory failure occurs
acutely, the situation is critical and hospital care is necessary.
R.J.G. – A Case of Respiratory Failure Due to COPD
Mr. G. first developed symptoms of lung disease at age 62, although by history he had a chronic productive cough for over 20 years. His main symptom was shortness of breath on exertion. Breathing tests confirmed emphysema with severe airway obstruction, and he was strongly advised to quit smoking. He tried, but the stress of business plus the heavy smoking by associates at sales meetings made it difficult; he continued to smoke at least a pack a day.
At age 64 he developed pneumonia and severe respiratory distress and was hospitalized. On admission to the hospital he was "blue" and confused; an arterial blood gas showed severe oxygen deficiency and a high CO2 tension in the blood. Because of this and his mental confusion he had to be artificially ventilated. Mr. G. was put in the intensive care unit, and a tube was placed in his throat (intubation) and connected to a ventilator. He had a stormy course, but after five days he was able to be disconnected from the ventilator. In another 10 days he was well enough to go home.
During his hospital convalescence he also resumed smoking, at first hiding the fact, but then smoking openly, despite repeated protestations by his family and his doctor. Pulmonary function studies done just prior to his discharge showed worse lung function than two years earlier; in addition his oxygen tension was low, but better than on his admission and not yet severe enough to warrant home oxygen therapy.
Mr. G. cut down his smoking to about half a pack a day. He was now severely limited and could walk no more than a block without disabling shortness of breath. He retired from his job. Two months after his 65th birthday he noted swelling of his feet and increased shortness of breath. His doctor diagnosed heart failure due to lung disease, prescribed water pills, and told him to quit smoking. Three months later he became somnolent, turned blue, and was quickly admitted to the hospital. His blood oxygen tension was again very low, with high carbon dioxide tension and increased blood activity. Initially treatment, was attempted with judicious amounts of oxygen and bronchodilators. However, Mr. G. continued to deteriorate; six hours after admission he had to be intubated and artificially ventilated. During this time he developed severe pneumonia, and despite antibiotics, oxygen, and various other medications, he died two days later.
An autopsy was performed. It revealed severe emphysema and bronchitis, the former predominating. In addition, his heart was enlarged from the stress of working against such damaged lungs. He had pneumonia in both lungs – the immediate cause of death.
This case represents the most severe
stage of COPD — low oxygen levels, heart failure, and death. Had
he stopped smoking at age 62 his downhill course might not have
been so precipitous; however, even at that age he already had
severe, far advanced disease. It takes years for this advanced
state to develop, yet during all that time he was asymptomatic
except for his daily cough. Had breathing tests been done, say
at age 50, they would have revealed some impairment in lung function.
Unfortunately, by the time his case was diagnosed it was endstage.
CAN ONE DEVELOP "ACUTE" EMPHYSEMA?
Emphysema, destruction of lung tissue, usually occurs over aperiod of years before symptoms develop; there is no counterpart to acute bronchitis, which can occur in otherwise healthy people. Some cigarette smokers (particularly those with alphalantitrypsin deficiency) can develop rapidly progressive emphysema leading from symptoms to death in less than a year, but this is very unusual.
Patients with emphysema may have such poor lung function
that anyadded insult makes them acutely ill. This could
be any lung infection.
ARE THERE DRUGS FOR EMPHYSEMA?
For pure emphysema there are no drugs available. The problem in pure emphysema is destruction of normal lung tissue, and no drugs can restore destroyed tissue. However, because most patients with emphysema also have some chronic bronchitis in the undestroyed portions of their lungs, the same modalities used to treat bronchitis are often used in emphysema patients. (Table 1)
Also, as previously mentioned, patients with emphysema
may develop some asthma as well. Because of co-existing asthma
and/or chronic bronchitis, many patients "with emphysema"
get treated with the same drugs used in those two conditions.
So, in summary, there are no drugs for emphysema, but there are
drugs for patients with emphysema.
WHAT ABOUT SURGERY FOR EMPHYSEMA?
Several surgical techniques have recently been developed to help patients with severe emphysema. These techniques don't actually treat the emphysema as much as remove unhealthy lung tissue and allow remaining lung tissue to expand. However, the operation is major surgery and not all patients can benefit. At this writing, it is too soon to know how effective this surgery will be over the long-term, as only a small number of patients have had it.
The technique is called "volume reduction surgery." At operation, segments of one or both lungs are removed which, on CT scan, appeared to be over-expanded and squeezing the "good" lung tissue. By removing these over-expanded areas, the surgeon hopes that remaining "good lung" can expand and provide more breathing surface to the patient.
Patients have definitely improved with this lung
surgery, and many have come off oxygen. However, patient selection
is critical because not all emphysema patients have the type of
disease that can benefit. The actual technique can be done with
a scalpel, as in traditional surgery, or with lasers. Any patient
with severe emphysema can be evaluated to see if surgery is recommended;
if so, he or she must inquire further about the potential benefit
and risks.
WHAT ABOUT FLU SHOTS AND THE PNEUMONIA VACCINE?
There are two recommended preventive vaccines for patients with COPD (as well as for other patients). Flu vaccine prevents infection with certain influenza viruses. Because the major flu virus changes yearly, the vaccine is updated annually to prevent infection with the current viral strain. The official Public Health Service recommendation is that any patient with chronic lung disease should receive the current flu shot. The basis for this recommendation is that the flu (a viral infection) affects the lungs and in compromised patients could be debilitating or even fatal.
In 1978 the Federal Drug Administration approved a pneumococcal vaccine for prevention of one common form of pneumonia caused by the bacteria pneumococcus (also known as streptococcus pneumoniae). There are approximately 70 strains of this bacteria that can cause pneumonia; the vaccine is designed to prevent infection with the 28 most virulent and potentially fatal. Pneumococcal organisms are also sensitive to penicillin, but elderly people and debilitated patients have lower host defenses against these organisms. For such patients (and some others) the vaccine is recommended once. At this writing repeat vaccination is not recommended unless the patient received an older version of the vaccine than is currently available.
Both the pneumococcal vaccine and the flu vaccine
may be given at the same time.
WHAT KIND OF LIFESTYLE CAN COPD PATIENTS LEAD?
The symptom that bothers most COPD patients is shortness of breath, or what doctors call dyspnea. It is dyspnea that COPD patients find most limiting, sometimes debilitating, and occasionally frightening. The "chronic" in COPD means the lungs won't rejuvenate – the disease will remain with the patient. Yet even for patients with severe disease much can be done to maintain or improve the quality of life. For the vast majority of COPD patients the answer to this question is "near normal and rewarding."
Pulmonary physicians are familiar with the following paradox. One patient with severe COPD is incapacitated, housebound, bitter, and angry. Nothing helps and life does not seem worth living. Another patient – with identical lung impairment – lives a full and rich life, stays involved in activities, and enjoys being alive. Both patients have respiratory limitation, but only one has learned to cope. Why the difference?
Some of the reasons may be beyond the capacity for patient or physician to change: differing degrees of family support, basic personality differences, unequal incomes, job status, and so forth. Even so, there are many things that can be altered and, as a result, markedly improve a COPD patient's quality of life.
To a large extent quality of life can be improved just by good medical care, including any necessary medications and correction of whatever reversible disease is present. Beyond this, the most obvious measure is to stop smoking. Cessation of smoking by itself may add enough oxygen to the blood to make the difference between breathing easily and still feeling short of breath. There is simply no excuse for any patient limited by lung disease to smoke. Period.
Also helpful is weight control. Although a discussion of weight loss is beyond the scope of this chapter, diet books (if needed) can be found in virtually every bookstore. Weight loss is obviously not easy (or there wouldn't be so many books); nonetheless, it can't be minimized — overweight patients feel better and breathe easier when they lose the extra pounds.
The combination of taking medications, stopping smoking, and losing weight can make a dramatic difference for many COPD patients. Of course, not all patients fit this picture. What about the patient who takes medication, has quit smoking and is not overweight, but is still limited by breathlessness? Such patients may benefit from oxygen therapy, a determination best made after a blood oxygen measurement.
Beyond these few points, there are other measures
that can improve the quality of an individual's life. The next
few sections – dealing with exercise, postural drainage, climate, sex, and travel – provide specific information that may be helpful for the COPD patient.
ARE BREATHING EXERCISES HELPFUL?
To a certain extent some breathing exercises are helpful in COPD. They help the patient only to breathe slightly more efficiently and perhaps feel more comfortable, but they do not alter the basic disease or improve lung function.
Patients with bronchitis and emphysema have trouble getting air out. In emphysema, the airways have a tendency to collapse from destruction of surrounding lung tissue. If patients purse their lips on exhalation to make a smaller mouth opening, the airways stay open a little longer and allow more time for the air to come out. This is called "pursed lip breathing" and is often practiced reflexively by patients with severe emphysema.
Another helpful exercise for both bronchitis and
emphysema patients is to take deep breaths and breathe out slowly,
i.e., avoid rapid breathing. This is particularly helpful for
patients who feel anxious over not being able to exhale fully;
if they remember to breathe slowly, they'll feel more comfortable.
WHAT IS PULMONARY REHABILITATION?
Pulmonary rehabilitation refers to a comprehensive program of physical training, diet control, and counseling for patients with severe COPD. Exercise training can definitely improve aerobic performance as well as the patient's sense of well being. Exercise training is usually done on a stationary bicycle or treadmill. Like breathing exercises, however, exercise training will not reverse damage to the airways nor significantly improve breathing capacity. There is still much to recommend in progressive exercise training, since it can improve overall cardiovascular fitness and make people feel better.
Of course, anyone with lung disease should undertake
exercise training only after first checking with his or her physician.
IS A WARM CLIMATE BETTER FOR PATIENTS WITH COPD?
There is no evidence that COPD patients, as a group, live healthier lives in a warm climate as opposed to a cold one. Obviously any patient who becomes sick from cold weather should consider a warmer place. But a substantial number of people have trouble breathing in hot, humid areas and prefer cooler weather. The decision to move (if that is involved) really has to be a personal one and cannot be based on a disease label. This is true for anyone with allergies and asthma as well as chronic obstructive pulmonary disease.
Many of the sun belt cities are heavily polluted,
the worst perhaps being Los Angeles. Altitude is another factor.
The higher the city, the less oxygen in the air; this makes Denver
a miserable place for patients with COPD and hypoxemia. As a general
recommendation anyone moving solely for health reasons should
research the area carefully and vacation there before deciding
on the move, preferably during the most extreme weather conditions
(for example, summer in Florida, winter in Minnesota).
WHAT ABOUT SEXUAL INTERCOURSE WITH COPD?
During sexual intercourse breathing effort is increased. For this reason patients with severe COPD (or any other chronic respiratory problem) may have difficulty during sex and may even avoid it because of anxiety about getting out of breath.
Sexual counseling for the respiratoryimpaired patient is little talked or written about. There is patient reluctance to complain to the doctor; doctor reluctance to broach such a sensitive area; and a general lack of information in medical journals. However, doctors recognize that COPD patients may have sexual problems related to their breathlessness, and that counseling can definitely help.
Probably the biggest obstacle to helping patients is uncovering the problem. The patient must let his doctor know and not simply wait to be asked (which may never happen). Once the sexual problem is aired, it is important to know if it is truly from shortness of breath or is instead an unrelated problem. Were there sexual difficulties before the onset of lung disease? Are there incompatibilities between the patient and his or her partner that have nothing to do with the lung disease? If so, specific psychological or marriage counseling may be needed.
Any sexual counseling for the COPD patient should include the sexual partner (as with anyone else). If the problem is due to shortness of breath, specific measures can be taken to help the patient accomplish – and enjoy – sexual intercourse.
Sexual intercourse is about as stressful as climbing a flight of stairs at a brisk pace, so shortness of breath during sex is acceptable if it can be tolerated. Despite the anxiety some patients have about dying during sex, sudden death is very uncommon during intercourse. Any steps that can be taken to prolong the sex act or make it more comfortable – unaccustomed positions (woman on top, for example), mutual masturbation, or prolonged foreplay – should be considered, tolerated and encouraged; as long as both partners find them acceptable.
Drugs commonly used to treat COPD should have no effect on sexual performance unless they cause side effects (such as fast heartbeat) at rest. In fact, use of an asthma-type inhaler just before sex may help prevent any shortness of breath. In addition, use of oxygen during intercourse is worth considering if it helps to relieve any shortness of breath. A nasal oxygen catheter can be unobtrusive and not interfere with the act of lovemaking. Drugs to be avoided are any central nervous system stimulants or depressants, since they may interfere with breathing and sexual function. Also, some antihypertensive medications may interfere with sexual function.
In summary, sex should not be a casualty of chronic
lung disease. Careful counseling and judicious use of medications
can go a long way in improving this important aspect of daily
living.
IS FLYING DANGEROUS FOR PATIENTS WITH COPD?
The answer to this question depends mainly on the patient's blood oxygen level before flying. If it is very low, flying may not be safe without extra or supplemental oxygen.
To explain further, consider what happens with altitude.Barometric or air pressure decreases with altitude. Although air pressure falls, the percentage of oxygen remains fixed – always 21% of the atmosphere at any altitude. However, 21% of a lower atmospheric pressure means less oxygen is in the air. For this reason mountain climbers often carry portable oxygen tanks at very high altitudes.
People living in Leadville, Colorado, the highest U.S. incorporated city, breathe 21% oxygen, but at a low barometric pressure; hence, they have a lower oxygen pressure in their blood than people in any other U.S. city. Healthy people in Leadville don't need to worry about this, because normal body mechanisms adapt to keep the total oxygen supply adequate. However, adaption takes time, and with a sudden ascent compromised people can experience difficulty.
The problem with flying is that airplane cabins are pressurized to an effective altitude of about 8,000 feet. When the captain says the plane is cruising at 30,000 feet, the air pressure inside is equivalent to 8,000 feet altitude – about half-way between the altitudes of Denver and Leadville. (Figure 6).
Problems at airline-cabin altitude may occur in people who have low oxygen tension in their blood. Although not everyone with COPD has low oxygen tension, severe COPD is the most common cause (called chronic hypoxemia).
This potential problem can easily be avoided by using oxygen during the flight. Most people who require oxygen during flight are those who also need it when not flying. Patients not on oxygen, but who think they might need it while flying, should consult their physician; the need can easily be determined by measurement of oxygen levels in the blood.
Arrangements for oxygen must be made in advance,
by informing the airline. The airline will require a physician's
prescription for the amount of oxygen required. Airlines provide
their own tanks for inflight use; these tanks are not
part of the oxygen system above every passenger seat; that
oxygen supply is only used in the event of sudden cabin decompression.
Figure 6. Flying in Airplane

WHAT IS THE FUTURE FOR CHRONIC OBSTRUCTIVE PULMONARY DISEASE?
Although our understanding and treatment of COPD
are more sophisticated than 20 years ago, there have been no dramatic
breakthroughs. We understand traditional drugs much better and
have a few new ones. But the basic disease is still chronic, and
patients with the condition still suffer. A cure is not on the
horizon. Once the damage is done the lung tissues do not regenerate
even when the insult (usually cigarette smoke) is removed. There
is no machine to take over breathing if our lungs fail completely,
such as dialysis for kidney failure. As far as lung transplantation,
this also is not feasible except for a very few end-stage patients.
Unfortunately, lungs are among the hardest organs to transplant,
much harder than kidneys and hearts. Patients receiving a lung
transplant must take large amounts of medication the rest of their
life. The worst aspect is that even when the operation is successful,
the transplanted lung begins to "wear out" after a few
years. Also, like all transplantable organs, lungs are however
hard to come by, requiring a fresh cadaver donor. At this writing
lung transplants, available in very few medical centers, can in
no way be considered a good treatment for endstage lung
disease.